Click for pdf: Elbow injuries
General presentation
Elbow injuries are extremely common in children. Upper extremity injuries account for 65% of injuries in children, of which fractures and dislocations of the elbow are the second most common. This high frequency is due to children being less skeletally mature than adults but also usually more active.
Anatomy, Epiphyseal Development and Elbow Ossification
The elbow joint is articulated proximally by the humerus and distally by the radius and ulna. Motion of the elbow is limited by complex bony anatomy and is kept stable by medial and lateral ligaments.
Understanding of the anatomy and development of the pediatric elbow is essential to accurate diagnosis and management of elbow injuries. The elbow joint itself is complex and is composed of 3 articulations:
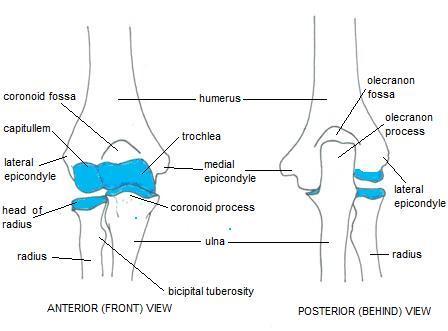
1. Ulnohumeral – between the trochlea of the humerus and the olecranon of the ulna
2. Radiohumeral – between the capitellum of the humerus and the radius
3. Radioulnar – between the proximal radius and the ulna
Figure 1: Elbow Anatomy. As distributed at http://www.joint-pain-expert.net/elbow-anatomy.html, used with permission.
The type of elbow injury depends on the anatomic and biomechanical properties inherent to the epiphyseal plate, musculotendinous units and articular cartilage, and to the specific injury. Both the age and sport of the patient can often predict the pathologic response. As such, epiphyseal development is critical in understanding the diagnosis. There are 6 growth centres within the elbow that appear in a consecutive manner. The mnemonic “CRITOE” allows for remembering the progression of ossification of the elbow’s secondary ossification centers:
- C – Capitellum (1 to 2 years)
- R – Radial epiphysis (3 to 4 years)
- I – Inner epicondyle (medial epicondyle, 5 to 6 years)
- T – Trochlea (9 to 10 years)
- O – Outer epicondyle (lateral epicondyle, >10 years)
- E – common Epiphysis (14 to 16 years years)
Each secondary ossification center appears as a single bony focus radiographically. Signs of potential injury involve variations in the size, density, position and number of secondary ossification centers.
Questions to ask
The history is especially important in assessing and evaluating elbow injuries. Localization, duration, character, temporal sequence, nature of onset, and activity level are all clues to the underlying pathology. The age of the child is also very important. Pain is the most common complaint, but other presenting complaints include decreased elbow motion, mild flexion contracture, swelling, decreased sport performance, and local sensitivity of the elbow.
History of Presenting Illness:
– Is there anything that makes the pain worse? (i.e. wrist flexion/pronation/extension)
– Is there anything that makes the pain better?
– Can you describe the pain? (dull vs. sharp)
– Does the pain radiate anywhere?
– Could you point exactly to the pain with one finger?
– When did you start noticing the pain?
– How long does the pain last? (an indirect measure of the severity)
– Any history of trauma?
– Do you play any sports? What kind? (baseball, tennis, gymnastics)
– Any associated symptoms (swelling, refusal to move arm)
Past Medical History:
– Have you had any previous surgeries? (Prior shoulder surgery may place the elbow at risk)
– Have you had any previous elbow injuries?
Family History:
– Any family history of osteochondritis?
Differential diagnosis
5 Common Types of Elbow Injuries
When evaluating the elbow, division of the examination into specific anatomic areas is critical.
Nursemaid’s Elbow (Subluxation of the Radial Head)
Nursemaid’s elbow is the most common elbow injury in children under 5 years of age and is unique to young children. It typically occurs when a longitudinal traction force is applied to the arm when the forearm is pronated and extended. This often occurs when a parent grabs the arm of a falling child or when the child is pulled by the hand. When this occurs, a portion of the annular ligament slips over the head of the radius where the ligament gets trapped in the radiohumeral joint. The child will usually cry immediately after the injury and will not use the affected arm, holding it limply in a slightly flexed and pronated position. Physical examination will also reveal radial head tenderness and resistance on attempted supination.
Treatment is a straightforward reduction where one places the thumb over the radial head, supinates the forearm and then flexes the elbow. One will often feel or hear a palpable click with reduction.
The annular ligament thickens and strengthens by 5 years of age and thus this injury is uncommon in older children.
Little League Elbow
Medial condylitis, or “Little League Elbow”, includes a constellation of abnormalities in young baseball pitchers resulting from shearing, inflammation, traction and abnormal bone development related to the stress of throwing. It is a valgus overload or over stress syndrome. Symptoms include swelling, pain, performance difficulties and weakness. Aggravation of symptoms results from wrist flexion and pronation. The number of pitches may be more important than the type pitch thrown in developing elbow injury. Those commonly presenting with medial condylitis are pitchers, infielders, catchers and outfielders (from most frequent to least frequent)
Panner Disease
Panner Disease is an abnormal ossification of the capitellum secondary to an idiopathic abnormal disturbance in blood flow in the bone that may allow collapse of the capitellum. It may also be the result of repetitive trauma leading to fragmentation and separation of bone and cartilage. It is common in children aged 5-12 years who engage in sports involving overhead throwing and arm weight bearing sports such as gymnastics. Children present with dull aches in the lateral elbow, aggravated by additional throwing. Presentation also includes swelling and reduced elbow extension. Radiographs show an abnormal capitellum, with fragmentation and areas of sclerosis.
Osteochondritis Dissecans
Osteochondritis dissecans (OCD) refers to an area of bone adjacent to articular cartilage that becomes avascular and eventually separates from the underlying bone. It is also a term for osteochondral fracture. The underlying etiology is unknown, but in children it may represent a disturbance in epiphyseal development in addition to repetitive trauma. OCD most commonly presents in the knee, but also in the elbow in the anterolateral aspect of the capitellum. It often presented in athletes aged 13-15 years and presents as lateral elbow pain, swelling, lack of full extension and occasional locking. Radiographs and MRI can fully demonstrate the lesion.
Lateral Epicondylitis
Lateral Epicondylitis is the most common sports injury of the elbow and accounts for 7% of all sports injuries. It presents in older children who participate in racket sports, as it results from the overuse of the extensor muscle in the forearm. It can also be seen in computer users from repetitive wrist extension. Children present with lateral elbow pain, which is aggravated by wrist extension and may radiate down the lateral forearm. There is usually pain on palpation of the lateral epicondyle which is exacerbated by resisted wrist extension.
Note: elbow pain may be a cause of referred pain from the shoulder or wrist.
Investigations
- Elbow radiographs, including comparison films: looking at secondary ossification centers
- Arthography
- Bone scans
- MRI studies
Conclusion
Elbow injuries are common in children, especially in athletes involving overhead throwing, racket sports and arm weight bearing activities. In the toddler, one should be familiar with the Nursemaid’s elbow. A thorough history and physical examination in addition with radiographical imaging if needed, will lead to appropriate diagnosis and management.
References
1. DeLee, J. C., Drez, D., and Millder, M. D. DeLee and Drez’s Orthopaedic Sports Medicine (3e). 2009.
2. Green, N. E., and Swiontkowski, M. F. Skeletal Trauma in Children (4e). 2009.
3. Hay, W. Levin, M. Deterding, R., and Sondheimer, J. Current Diagnostic and Treatment Pediatrics (19e). 2008.
4. Chorley, J. Elbow injuries in the young athlete. UpToDate 2011. www.uptodate.com.
5. Kleigman et al. Nelson’s Textbook of Pediatrics 18th Edition. Chapter 680: Upper Limb. Saunders Elselvier 2007.
Acknowledgements
Written by: Gilbert Lam
Edited by: Anne Marie Jekyll, MD (Pediatric Resident)


 (12 votes, average: 4.08 out of 5)
(12 votes, average: 4.08 out of 5)