Click for pdf: ECG basics
First thing’s first
- Check the name on the top of the ECG – is this your patient?
- Check the date – is this the one you ordered?
- Check for old ECGs – just like a chest xray, it’s always a good idea to compare with an old one
- Check for the age of the patient – the heart physiology and the normal values differ in different age groups in the pediatric population
Note: You may want to cover the top part of the ECG sheet now. Do not rely on the computer calculated numbers; it may be wrong. Trust yourself!
Technical Aspects
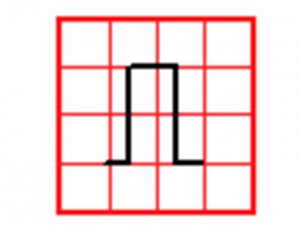
- Is the ECG full standard?
- Full standard means that the ECG was not reduced in size so that it can fit on the paper
- Look at the left hand side of each line
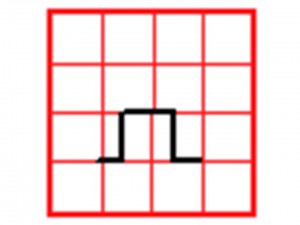
If it is full standard, the rectangle’s height should be 2 big squares
If it is half standard, the rectangle’s height is only 1 big square. You will need to double all the waves to normalize them
What is the paper speed?
- The standard speed is 25mm/sec
- That means each little box is 0.04 seconds, each big box is 0.2 seconds, the whole strip is 6 seconds
- Now look at the top of the ECG, there should be a print out of what speed the ECG was ran at
- For tachyarrhythmias, the speed of the ECG may have been increased to 50 mm/sec in order to visualize the p waves; in this case, the speed and duration of the ECG components will need to be doubled
Rate
- Normal, Fast or Regular Rates
- Find 2 adjacent R waves, count the number of big squares between the R’s
- Divide 300 by the number of big squares : this is your rate
- Or . . . .Find a QRS complex that starts on a thick line, then count the thick lines using these numbers “300-150-100-75-60-50” to the next QRS
Slow or Irregular Rates
- The easiest way to calculate the rate is to count the total number of QRS complex along the length of the entire strip and multiply it by 10: this is your rate (bpm)
- Note: The normal value for heart rate ranges dramatically depending on your patient’s age. Please compare your patient’s age and heart rate with Table 1.
Rhythm
Analysis
- Is the rhythm sinus?
Sinus rhythm:
- Is there a P wave before each QRS complex?
- Is there a QRS complex after every P wave?
- Are the P waves upright in leads I, II, III?
- Do all P waves should look the same?
- Are all P wave axis normal (0° to +90°)?
- Are the PR intervals constant?
- Is the rhythm fast or slow? (refer to Table 1 values)
- Is the rhythm regular or irregular? Do the P waves and QRS follow a regular pattern?
- If it is irregular, is it consistently irregular or consistently irregular?
Consistently irregular = some form to the pattern of irregular complex i.e. predictable
Inconsistently irregular = no pattern at all i.e. unpredictable
Abnormal Rhythms
| Premature Atrial Contraction (PAC) |
|
| Premature Ventricular Contraction (PVC) |
|
| Atrial Flutter |
|
| Atrial Fibrillation |
|
| Ventricular Tachycardia |
|
| Ventricular Fibrillation |
|
Axis
- Axis is the “conduction flow” of the heart
- Normal axis varies with age – i.e. newborns have a right axis deviation because the left and right ventricles are the same size due to fetal circulation
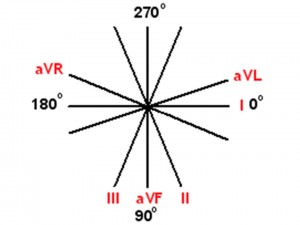
- Look at the QRS complex of Lead I and Lead aVF
- Is the QRS complex of Lead I more negative (downgoing or conduction away from the lead) or positive (upgoing or conduction towards the lead)?
- Is the QRS complex of Lead aVF more negative or positive?
| Lead I | Lead aVF | Axis |
| + | + | Normal |
| + | – | Left Axis Deviation |
| – | + | Right Axis Deviation |
| – | – | Extreme Right Axis Deviation |
P Wave and PR Interval
- PR = beginning of P to beginning of QRS
- P wave normal is 2-3 little squares (0.08-0.12); if wide P wave = left atrial enlargement
- If P wave is taller than 2-3 little squares = right atrial enlargement
- PR interval is dependent on age (Table 1); if PR is wide = first degree AV block
QRS Complex
- If beginning of Q to end of S is longer than 2-3 small squares: bundle branch block
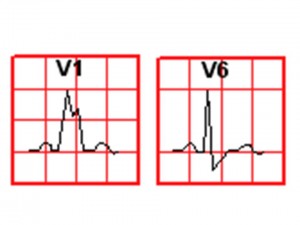
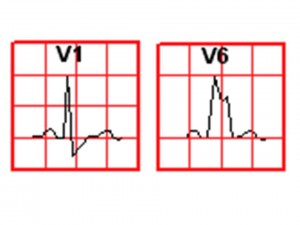
- Look for the “M” sign in either V1 or V6
- If the “M” is on V1: Right bundle branch block (RBBB)
- If the “M” is on V6 : Left bundle branch block (LBBB)
QTc Interval
- Beginning of Q to end of T
- QT corrected interval for heart rate because as HR decrease, QT lengthens and vice versa
- Normal: <0.45 (<6 months), <0.44 (>6 months)
- QTc = QT / square root of RR interval
- DDx prolonged QT: long QT syndrome, hypokalemia, hypomagnesemia, hypocalcemia, neurologic injury
- Prolonged QT predisposes to ventricular tachycardia and associated with sudden death
T wave
- DDx of peaked, pointed T = hyperkalemia, LVH
- DDx of flattened T waves = hypokalemia, hypothyroidism
Ventricular Hypertrophy
Right ventricular hypertrophy
If any of the following:
- R wave >98% in V1 or S wave >98% in I or V6
- Increased R/S ratio in V1 or decreased R/S in V6
- RSR’ in V1 or V3R in the absence of complete RBBB
- Upright T wave in V1 (>3 days)
- Presence of Q wave in V1, V3R, V4R
- DDx of RVH: ASD, TAPVR, pulmonary stenosis, TOF, large VSD with pulmonary HTN
Left ventricular hypertrophy
If any of the following:
- R >98% in V6, S >98% in V1
- Increased R/S ratio in V6 or decreased R/S in V1
- Q >5mm in V6 with peaked T
- DDx: VSD, PDA, anemia, complete AV block, aortic stenosis, systemic HTN
Appendix
a) Table 1: Normal Values
| Age | HR bpm |
QRS axisdegrees |
PR intervalseconds |
QRS intervalseconds |
R in V1mm |
S in V1mm |
R in V6mm |
S in V6mm |
| 1st week | 90-160 | 60-180 | 0.08-0.15 | 0.03-0.08 | 5-26 | 0-23 | 0-12 | 0-10 |
| 1-3wks | 100-180 | 45-160 | 0.08-0.15 | 0.03-0.08 | 3-21 | 0-16 | 2-16 | 0-10 |
| 1-2 mo | 120-180 | 30-135 | 0.08-0.15 | 0.03-0.08 | 3-18 | 0-15 | 5-21 | 0-10 |
| 3-5 mo | 105-185 | 0-135 | 0.08-0.15 | 0.03-0.08 | 3-20 | 0-15 | 6-22 | 0-10 |
| 6-11 mo | 110-170 | 0-135 | 0.07-0.16 | 0.03-0.08 | 2-20 | 0.5-20 | 6-23 | 0-7 |
| 1-2 yr | 90-165 | 0-110 | 0.08-0.16 | 0.03-0.08 | 2-18 | 0.5-21 | 6-23 | 0-7 |
| 3-4 yr | 70-140 | 0-110 | 0.09-0.17 | 0.04-0.08 | 1-18 | 0.5-21 | 4-24 | 0-5 |
| 5-7 yr | 65-140 | 0-110 | 0.09-0.17 | 0.04-0.08 | 0.5-14 | 0.5-24 | 4-26 | 0-4 |
| 8-11 yr | 60-130 | -15-110 | 0.09-0.17 | 0.04-0.09 | 0-14 | 0.5-25 | 4-25 | 0-4 |
| 12-15 yr | 65-130 | -15-110 | 0.09-0.18 | 0.04-0.09 | 0-14 | 0.5-21 | 4-25 | 0-4 |
| > 16 yr | 50-120 | -15-110 | 0.12-0.20 | 0.05-0.10 | 0-14 | 0.5-23 | 4-21 | 0-4 |
References
Garcia, Tomas and Neil Holtz. 12-Lead ECG: The Art of Interpretation. Jones and Bartlett Publishers Canada. 2001
Interpreting Pediatric ECG. Pediatric Cardiology at the University of Chicago. http://pediatriccardiology.uchicago.edu/MP/ECG/ECG-submenue.htm
Acknowledgments
Written by: Jasmine Lam
Edited by: Jeff Bishop


 (17 votes, average: 4.41 out of 5)
(17 votes, average: 4.41 out of 5)
an excellent presentation,learning and a tremendous website.
BEST